|
SEXUALITY
AND SPINAL CORD INJURY
by
Stanley Ducharme, Ph.D.
Reprinted
from: The Rehabilitation of People With Spinal Cord Injury,
Second Edition, Blackwell Science Publishers, Boston, 2000
INTRODUCTION
With longer life expectancies following SCI, the emphasis
in rehabilitation over the past decade has gradually shifted
to improved quality of life. Toward this goal, issues related
to sexuality must be addressed by the rehabilitation team
in both the acute and chronic stages of SCI. Providing sexual
education to patients and their partners is best accomplished
by an interdisciplinary team approach in which medical and
psychological issues can be addressed.
MALE
SEXUAL ACT
Erectile and ejaculatory function are complex physiological
activities that require the interaction between the vascular,
nervous and endocrine systems. Erections are controlled
by the parasympathetic nervous system.
In
the simplest of terms, erection is controlled by a reflex
arc that is mediated in the sacral spinal cord. A reflex
involves an afferent and efferent limb. The afferent limb
consists of somatic afferent fibers from the genital region
that travel through the pudental nerve into the sacral spinal
cord. These fibers travel through the cauda equina and exit
via the S2 to S4 nerve roots. The post-ganglionic parasympathetic
fibers secrete nitric oxide, which causes relaxation of
the smooth muscle of the corpus cavernosum and increases
blood flow to the penile arteries. Consequently, the vascular
sinusoids of the penis become engorged with blood and the
result is an erection. This reflex is modulated by higher
brainstem, subcortical and cortical centers. In addition,
erectile function is influenced by hormonal factors such
as testosterone.
Ejaculation
signals the culmination of the male sexual act and is primarily
controlled by the sympathetic nervous system. Similar to
the sympathetic innervation of the bladder, these fibers
originate in the thoraco-lumbar spinal cord and travel into
the sympathetic chain. These fascicles then travel through
the splanchnic nerves into the hypogastric plexus. After
synapsing in the inferior mesentericganglion, postganglionic
fibers travel through the hypogastric nerves to supply the
vas deferens, seminal vesicles and ejaculatory ducts in
the prostate.
FEMALE
SEXUAL ACT
The physiology of the female sexual act has not been studied
as well as the male sexual act. However, female sexual satisfaction
is dependent on a complex interaction of the endocrine and
nervous systems. Sexual excitation is the result of psychogenic
and physical stimulation. This arousal is manifested by
vaginal lubrication and tightening of the interoitus. Stimulation
of the genital region including the clitoris, labia majora
and labia minora causes afferent signals to travel via the
pudendal nerve into the S2 to S4 segments of the spinal
cord. These fibers interact with efferent parasympathetic
fibers that project through the pelvic nerve. The result
is dilation of arteries to perineal muscles and tightening
of the interoitus. In addition, the parasympathetic fibers
cause the Bartolin’s glands to secrete mucus, which
aids in vaginal lubrication.
Female
orgasm is characterized by the rhythmic contraction of the
pelvic structures. Female orgasm also results in cervical
dilation, which may aid in sperm transport and fertility.
SEXUAL
HISTORY
A simplified sexual history should be part of the initial
clinical assessment. Key elements include physical capabilities,
past sexual activities and current sexual function. In addition,
the clinician should inquire into the partner’s availability,
partner satisfaction, sexual orientation, behavioral repertoire
and past sexual abuse. Open ended questions will facilitate
better communication. Topics of a more sensitive nature
should be reserved for later in the interview when a therapeutic
relationship has been established.
PSYCHOLOGICAL
CONSIDERATIONS
Adaptation to an SCI is a gradual process that extends over
a prolonged period of time. Successful sexual adjustment
is influenced by many factors such as age at time of injury,
quality of social supports, physical health, gender and
severity of the injury. Losses need to be mourned so that
the remaining strengths can be nurtured and developed. To
achieve satisfying sexual adjustment, a person with an SCI
will have to learn their new sexual abilities, as opposed
to recapturing the past.
After
a traumatic injury, individuals typically go through a period
of reduced sexual drive. Although libido is not affected
by SCI, it may be diminished by depression, trauma of the
injury or medications. Initially after injury, some persons
with SCI may deny the importance of sexual issues. Other
individuals may be reluctant to discuss issues related to
sexuality due to cultural or personal reasons. Other patients
may go through a period of sexual “acting out”
(i.e., unacceptable sexually explicit language, inappropriate
unwanted physical contact with staff, etc.) while on the
rehabilitation unit.
During
the acute rehabilitation phase, a sensitive discussion regarding
sexuality is appropriate. The person with SCI may inquire
about issues such as dating, attractiveness, relationships,
parenthood and physical appearance. Other topics of interest
may include erections, lubrications, sensation, orgasm,
ejaculation and fertility. Many individuals will inquire
about sexuality as it related to bladder and b function.
Even if the patient does not initiate discussions about
these topics, it is important for members of the rehabilitation
team to provide basic information.
MALE
AND FEMALE AROUSAL
Men and women with SCI often lack sensation at traditional
erogenous areas such as the genitals and nip. As such stimulating
these areas may result in penile erections or vaginal lubrication
but not necessarily sexual pleasure. However, other areas,
sometimes not normally recognized as erogenous areas, such
as the ears, eyelids and neck, can be stimulated to provide
sexual arousal. Some individuals find the skin surface around
the neurological level to have heightened tactile sexual
response.
MALE
SEXUAL FUNCTION: ERECTIONS, EJACULATION AND ORGASM
Men with SCI may obtain reflexogenic or psychogenic erections.
Reflex erections are secondary to manual stimulation of
the genital region. Psychogenic erections are the result
of erotic stimuli that result in cortical modulation of
the sacral reflex arc. In general, erections are more likely
with incomplete injuries (both upper and lower motor neuron),
than complete injuries. Many times, men with SCI can only
maintain an erection while the penis is stimulated and the
quality of the erection is insufficient for sexual satisfaction.
As such, the erection must be augmented with devices, medications
or a penile implant for satisfactory sexual function.
In
men with SCI, the ability to ejaculate is less common than
the ability to obtain an erection. The rate of ejaculation
varies depending on the nature and location of the neurological
injury. In complete upper motor neuron lesions, the ejaculation
rate is estimated at 2 percent. In incomplete upper motor
neuron lesions, the ejaculation rate is estimated to be
somewhat higher at 32%. Many men who are able to ejaculate
experience retrograde ejaculation into the bladder, some
may experience dribbling of semen.
The
experience of orgasm in men with SCI is variable. Some individuals
describe a primarily emotional event. Others experience
generalized muscle relaxation or a pleasant sensation in
the pelvis or at the sensory level. Other men report orgasm
to be non-existent following the injury.
ORAL
THERAPY FOR MALE SEXUAL DYSFUNCTION
Sildenafil (Viagra) was approved by the FDA in 1998, and
may have a significant role in the treatment of erectile
dysfunction for men with SCI. Sildenafil is a type 5 phosphodiesterase
inhibitor that prevents the intracorporal breakdown of cyclic
GNP. It is rapidly absorbed after oral administration and
is taken approximately 60 minutes before anticipated sexual
activity. It is most effective for men who are capable of
achieving reflex erections. It can assist the man in gaining
further rigidity and in sustaining the erection for penetration.
Sildenafil is contraindicated in men taking nitrates due
to the risk of profound hypotension. Many men with SCI have
low baseline blood pressure and this agent should be prescribed
with caution. In addition, this drug is not recommended
for those individuals with cardiac disease. Side effects
noted in this otherwise well population include facial flushing,
dyspepsia, headache and visual disturbances.
INTRACAVERNOSAL
INJECTION THERAPY
 |
|
Intracavernosal
Injection Therapy
|
Therapy
with intracavernosal injection of papaverine, alprostadil
and phenotolamine is an accepted treatment of erectile dysfunction.
Initiating this therapy necessitates a referral to a urologist.
Initially, individuals are given small doses of the pharmacological
agent and the dose is increased until a satisfactory erection
is obtained for intercourse. Sometimes, a mixture of agents
is prescribed. Erections should not persist beyond four
hours. Many tetraplegics have impaired hand function and
will require a cooperative partner to perform the injection.
In some cases a commercially marketed penile autoinjector
can be easier to manipulate. Priapism is a possibility;
therefore, both partners should be properly trained. Some
individuals with incomplete injuries may experience pain
at the injection site.Penile fibrosis is also a potential
risk of intracavernosal therapy.
TRANSURETHRAL
THERAPY
Recently, transurethral delivery systems for administering
agents that result in erections have been approved. The
medication delivered is usually alprostadil. This treatment
is generally not as effective as intracavernosal therapy.
Many men are not satisfied with the rigidity of the erections
obtained.
PENILE
VACUUM DEVICES
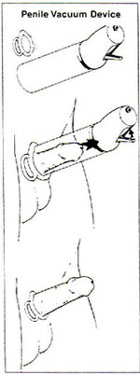 These
devises create a vacuum around the penis. As a result, blood
isdrawn into the corporal spaces. A band is then slipped
off the plasitic cylinder around the base of the penis to
maintain penile tumescence. Ejaculation may be retarded
due to the constriction of the urethrea. However, newer
models are available with constricting bands that are less
likely to diminish ejaculation. These
devises create a vacuum around the penis. As a result, blood
isdrawn into the corporal spaces. A band is then slipped
off the plasitic cylinder around the base of the penis to
maintain penile tumescence. Ejaculation may be retarded
due to the constriction of the urethrea. However, newer
models are available with constricting bands that are less
likely to diminish ejaculation.
Vacuum
devices are non-invasive, economical and efficacious. Howver,
these devices require some degree of manual dexterity. For
many men with tetraplegia, the partner must be willing to
assist with the procedure. In addition, men must transfer
out of the wheelchair and be in a recumbent position to
obtain a good vacuum seal at the base of the penis. Individuals
with incomplete injuries may experience pain, discoloration
and coldness at the base of the penis. Constriction rings
should not remain in placefor more than 30 minutes. Longer
time periods may be associated with potential skin breakdown.
Vacuum devises are more accepted by men in more established
sexual relationships. Some men use vacuum devices to augment
erections obtained with oral medications. Vacuum devises
are commonly used in underdeveloped nations where phramacotherapy
is unavailable or not affordable.
PENILE
IMPLANTS
Penile implants are considered when other treatments have
been  unsuccessful,
especially if trauma has disrupted the penile vascular system.
It also may be indicated is severe Peyronie’s disease
is a factor. Implants are not considered in the first year
post injury so that persons with SCI can make emotional
adaptations to the injury and explore less invasive options
for sexual activity. There are a number of different devises,
ranging from the simple malleable prosthesis to more complex
hydraulic prostheses. Generally, the choice of prosthesis
is related to individual preference and financial constraints. unsuccessful,
especially if trauma has disrupted the penile vascular system.
It also may be indicated is severe Peyronie’s disease
is a factor. Implants are not considered in the first year
post injury so that persons with SCI can make emotional
adaptations to the injury and explore less invasive options
for sexual activity. There are a number of different devises,
ranging from the simple malleable prosthesis to more complex
hydraulic prostheses. Generally, the choice of prosthesis
is related to individual preference and financial constraints.
MALE
FERTILITY
The ability to father a child correlates with the frequency
of ejaculation. Successful pregnancy rates range from 10
percent to 35 percent. In general, men with incomplete lesions
(both upper and lower motor neuron) are more likely to become
fathers than those with complete lesions. Conditions that
may contribute to infertility include retrograde ejaculation,
repeated urinary tract infections and altered testicular
temperature. Newer methods of obtaining semen samples include
rectal electroejaculation or penile vibroejaculation. Both
of these techniques may precipitate autonomic dysreflexia.
FEMALE
SEXUAL FUNCTION: SEXUAL AROUSAL AND VAGINAL LUBRICATION
Most women with SCI can achieve some level of vaginal lubrication.
This lubrication can be mediated by reflexogenic or psychogenic
factors. Individuals with incomplete (both upper and lower
motor neuron) injures are more likely to have satisfactory
lubrication. If vaginal lubrication is unsatisfactory, then
a water soluble lubricant can be recommended. Sildenafil
may be of value in women with SCI by increasing blood flow
to the perineum and increasing vaginal lubrication. , which
may improve sexual satisfaction. However, there are no controlled
studies on the female SCI population.
FEMALE
FERTILITY
Immediately after injury, 44 percent to 58 percent of women
suffer from temporary amennorhea. Menstruation usually returns
within 6 months post injury. Neither the level nor the completeness
of the injury appear to be associated with the interruption
of menstrual cycles. In a small percentages of women with
SCI, there are also changes in cycle length, duration of
flow, amount of flow and amount of menstrual pain. Most
women with SCI are fertile.
BIRTH
CONTROL
The issue of birth control can be somewhat problematic for
women with SCI. Condoms provide contraception as well as
diminish the risk of transmission of sexually transmitted
diseases. A diaphragm may be another acceptable option if
the individual has adequate hand dexterity or a cooperative
partner. Oral contraception is associated with increased
incidence of thromboembolism and must be prescribed with
caution in women with SCI. Oral contraceptives that contain
only progesterone may be safer than medications that contain
both estrogen and progesterone. IUD may be associated with
increased incidence of pelvic inflammatory disease . Untreated
PID may lead to autonomic dysreflexia. In addition, women
with SCI may not be able to perceive if the devise has migrated
out of the cervix.
PREGNANCY
Pregnant women with SCI have an increased risk of urinary
tract infections, leg edema, autonomic dysreflexia, constipation,
thromboembolism and pre-mature birth. Since uterine innervation
arises from the T10 to T12 levels, patients with lesions
above T10 may not be able to perceive uterine contractions
or fetal movements. It may be difficult to differentiate
between pregnancy induced hypertension (pre-eclampsia) and
autonomic dysreflexia. Autonomic dysreflexia may be the
only clinical manifestation of labor. During the second
and third trimester, pregnant women may have difficulty
in performing functional tasks that were previously completed
independently. Transfers may require the assistance of a
caregiver and a power wheelchair may be necessary for mobility.
Locating an obstetrician and anesthesiologist with a supportive
attitude, an accessible office and experience in SCI can
be difficult in many areas.
URINARY
AND FECAL INCONTINENCE
Urinary and fetal incontinence at inopportune times and
subsequent social rejection are major fears of some people
with SCI. A bladder or bowel accident may occur at any time
during courtship, sexual activity or during social events.
The embarrassment, shame and humiliation associated with
incontinence create undue anxiety and are often regarded
as a major reason for social isolation or the termination
of a relationship.
To
minimize untimely episodes of incontinence, the bladder
should be emptied prior to sexual activity. Foley catheters,
if present, can be taped to the side of the penis with a
condom placed over the catheter. Females can engage in sexual
intercourse despite the presence of a Foley catheter by
taping the catheter to the abdomen. Despite the best management
program, sexual stimulation can cause urinary and or fecal
incontinence . Embarrassing passage of gas from the vagina,
bowel or ostomy bag can be avoided by gentle thrusting,
coital positioning and a careful diet. Fluids should be
limited during the hours preceding sexual activity. Towels
should be available to manage episodes of urinary or fecal
incontinence.
CONCLUSION
Sexual adaptation after an SCI is a gradual process that
involves psychological and physical adjustments. The availability
of new medications, devices and procedures have greatly
enhanced the possibility of having a satisfactory sexual
life after an SCI. Toward this end, the rehabilitation team
has a responsibility to provide sexual information and counseling
during the acute and chronic stages of SCI.
SUGGESTED
READINGS
Boller, P. and Frank, E. Sexual Dysfunction in Neurologic
Disorders, New York, Raven Press; 1982.
Ducharme,
S. and Gill, K. Sexuality After Spinal Cord Injury, Baltimore,
MD, Paul Brooks Publishing Company; 1997.
Leyson,
J. Sexual Rehabilitation of the Spinal Cord Injured Patient.
Clinton, NJ; Humana Press, 1991.
Sipski,
M. and Alexander, C. Sexual Function In People With Disability
and Chronic Illness. Gaithersburg, MD; Aspen Publications;
1997.

Back
to Articles
|

